
Relationship Between Elevated Hair Mercury Levels, Essential
Element Status, and Metabolic Profile in Overweight
and Obese Adults
Anatoly V. Skalny
1,2,3
& Jung-Su Chang
4
& Igor P. Bobrovnitsky
5
& Philippe Yu Kopylov
1
& Margarita G. Skalnaya
6
&
Shih-Yi Huang
4
& Monica Maria Bastos Paoliello
7,8
& Ekaterina S. Ivanova
9
& Weu Wang
4
& Alexey A. Tinkov
1,2
Received: 12 August 2020 / Accepted: 8 October 2020
#
Springer Science+Business Media, LLC, part of Springer Nature 2020
Abstract
The objective of the present study was to evaluate hair essential and trace element levels and metabolic risk markers in
overweight and obese subjects in relation to body mercury burden. According to 2 × 2 factorial design a total of 440 adults were
distributed to four groups: (i) low-Hg normal-weight subjects (n = 114); (ii) high-Hg normal weight subjects (n = 113); (iii) low-
Hg overweight (BMI > 25) subjects (n = 110); (iv) high-Hg overweight (BMI > 25) subjects (n = 110). Hg-exposed groups
consisted of subjects characterized by frequent seafood consumption (> 4 times/week) subsequently evaluated by hair analysis
(> 0.58 μg/g). Dietary-exposed subjects were characterized by a more than 3-fold higher hair Hg content irrespectively of body
weight values. Both low-Hg and high-Hg overweight subjects were characterized by significantly higher ALT activity, as well as
elevated serum glucose, LDL, and triglyceride levels as compared to the respective groups of normal weight subjects. High Hg
body burden had a more significant effect on metabolic parameters in overweight and obese adults. Particularly, high-Hg
overweight subjects were characterized by significantly higher serum creatinine and uric acid levels, as well as increased GGT
and CK activity as compared to low-Hg overweight counterparts. In addition, hair Mg, Mn, and Sr content in high-Hg overweight
subjects was significantly lower than that in low-Hg normal weight and overweight examinees. In turn, high Hg levels in
overweight subjects were associated with significantly higher hair Se and Zn levels when compared to unexposed overweight
adults. Generally, the obtained data demonstrate that increased hair Hg levels in overweight and obese subjects is associated with
adverse metabolic profile. It is proposed that observed metabolic alterations may be at least partially mediated by Hg-associated
disturbances in essential trace element and mineral metabolism.
Keywords Mercury
.
Metabolic risk
.
Magnesium
.
Zinc
.
Gamma-glutamyl transferase
Introduction
Obesity is considered as a worldwide epidemic that raised
drastically during the last 50 years reaching the mean preva-
lence of up to 19.5% worldwide in 2015 [1]. Although posi-
tive caloric balance due t o increased food intake and low
energy expenditure is the primary cause of obesity, certain
other factors including the environmental ones may also con-
tribute to increased risk of obesity [2]. In 2002, Baillie-
Hamilton proposed the association between chemical toxin
exposure and obesity epidemic [3]. Since then multiple studies
demonstrated the potential contribution of a variety of organic
* Anatoly V. Skalny
skalny3@microelements.ru
1
I. M. Sechenov First Moscow State Medical University (Sechenov
University), Moscow 119146, Russia
2
Yaroslavl State University, Yaroslavl 150000, Russia
3
ITMO University, St. Petersburg 197101, Russia
4
Taipei Medical University, Taipei, Taiwan
5
Centre for Strategic Planning, Russian Ministry of Health,
119435 Moscow, Russia
6
Micronutrients Ltd., Moscow, Russia
7
Department of Molecular Pharmacology, Albert Einstein College of
Medicine, Bronx, NY 10461, USA
8
Graduate Program in Public Health, Center of Health Sciences, State
University of Londrina, Londrina, PR 86038-350, Brazil
9
National Medical Research Center for Therapy and Preventive
Medicine of the Ministry of Health of Russia, Moscow, Russia
Biological Trace Element Research
https://doi.org/10.1007/s12011-020-02430-2

compounds, mainly persistent organic pollutants, in the path-
ogenesis of obesity [4]. Despite the observed association be-
tween metal exposure and obesity [5], data on the potential
role of toxic metals as obesogens are scarce [6].
Multiple studies demonstrated a significant association be-
tween mercury (Hg) body burden and increased BMI [7, 8],
adiposity [9], and metabolic syndrome [10], although certain
contradictions exist [11]. Therefore, it is proposed that Hg
may contribute to obesity and metabolic syndrome pathogen-
esis through its impact on adipose tissue, insulin signaling,
energy, lipid, and carbohydrate homeostasis [12, 13].
Correspondingly, a recent study demonstrated that Hg expo-
sure is associated with adverse metabolic profile in obesity
[14]. However, data on the relationship between Hg body
burden in obesity and metabolic risk are insufficient.
In parallel with mercury, essential trace elements and min-
erals are also involved in obesity and metabolic syndrome
through their physiological functions [15]. Particularly, zinc
[16 ], chromium [17], and vanadium [18] are known to be in-
volved in insulin signal transduction. Selenium is also consid-
ered as an important regulator of adipogenesis and adipocyte
physiology [19]. Magnesium possesses antiinflammatory and
antioxidant effect in obesity [20]. Correspondingly, altered es-
sential trace element and mineral metabolism was shown to be
associated with obesity and metabolic syndrome [21–23].
Along with multiple mechanisms of Hg toxicity, it is also
known to interfere with essential metal metabolism through
competitive binding to metalloproteins [24]ordirectinterac-
tion with selenol groups [25]. Correspondingly, experimental
studies demonstrated that Hg exposure may result in alteration
of essential element homeostasis resulting in alteration of their
target functions [26, 27]. However, human data on the poten-
tial role of Hg-associated disturbances in trace element and
mineral metabolism in obesity and metabolic syndrome are
insufficient.
Therefore, the objective of the present study was to evalu-
ate essential and trace element levels in hair, and metabolic
risk markers in overweight and obese subjects in relation to
body mercury burden.
Materials and Methods
The experimental procedures were performed in agreement
with the ethical standards of the Declaration of Helsinki and
its later amendments. All examinees were informed about the
procedures and signed the informed consent form prior the
investigation. The protocol of the present study was approved
by the local ethics committee (Yaroslavl State University,
Yaroslavl, Russia).
A total of 440 adults participants were enrolled in the cur-
rent study. The study involved a 2 × 2 factorial design with
grouping according to BMI values and hair Hg content. Given
that seafood intake is the primary cause of Hg exposure, the
first selection approach to group participants was based on the
individuals’ frequency of seafood consumption (> 4 times/
week). Based on subsequent ICP-MS analysis, only seafood
consumers with hair Hg concentrations > 0.58 μg/g, estimated
as the cutoff of environmental Hg exposure [28], were includ-
ed in the study. The subjects were recruited at the Center for
Biotic Medicine (Moscow, Russia). The groups were defined
as follows:
Group I (n = 114)—low-Hg normal-weight subjects
(controls). Median and IQR for BMI = 21.8 (20.2–23.4)
kg/m
2
Group II (n = 113)—high-Hg normal weight subjects.
Median and IQR for BMI = 21.8 (20.6–23.1) kg/m
2
Group III (n = 110)—low-Hg overweight (BMI > 25)
subjects. Median and IQR for BMI = 28.1 (26.3–30.5)
kg/m
2
Group IV (n = 110)—hig h-Hg overweight (BMI > 25)
subjects. Median and IQR for BMI = 27.5 (26.2–29.7)
kg/m
2
No significant group difference in age or gender of the
examinees were observed (Table 1). However, in view of
certain age and gender variability, all comparisons were ad-
justed for age and gender. Body mass index (BMI) was eval-
uated using the obtained data on body height (m) and weight
(kg) according to the formula (BMI = body weight (kg)/
height
2
(m
2
)).
The examinees were interviewed to obtain information
about dietary habits (specific food habits including frequency
of fish consumption), occupation, smoking status, frequency
of alcohol consumption, city of origin, as well as duration of
living in Moscow. Questions on the use of hair dyes as well as
specific trace element enriched shampoos were also included.
In order to reduce the influence of confounding factors on
the analyzed variables, the following exclusion criteria were
applied: occupational Hg exposure in heavy metal industry;
smoking (current and former smoker status); using trace
element–enrich formulations as hair shampoos or other
haircare products; trace element and mineral supplementation;
metal implants; acute inflammatory diseases.
Venous blood samples were obtained after an overnight
fasting from the cubital vein using anticoagulant-free
“Vacuette” tubes (Greiner Bio-One International AG, 4550
Kremsmünster, Austria). Blood samples were subsequently
subjected to centrifugation at 1600g for 10 min to separate
serum. Only serum samples without hemolysis were used
for analysis.
Blood serum was analyzed for glucose, lipid spectrum, as
well as metabolic risk markers using the respective Randox
(Randox Laboratories Ltd., Crumlin, UK) kits at Tokyo Boeki
(Tokyo Boeki Machinery Ltd., Tokyo, Japan) biochemical
Skalny et al.

analyzer. Lipid spectrum was evaluated through assessment of
serum total cholesterol (TC), low (LDL-C), and high-density
lipoprotein cholesterol (HDL-C), as well as triglyceride (TG)
levels. Serum activity of alanine (ALT) and aspartate amino-
transferases (AST) [29], gamma-glutamyltransferase (GGT)
[30], as well as levels of creatinine [31], urea, and uric acid
(UA) concentration [32] were used as metabolic risk markers.
Hair samples were collected from occipital region in a
quantity of 0.1 g using ethanol-precleaned stainless steel scis-
sors. The collected samples were subjected to washing with
acetone a nd subsequent rinsing distilled deionized water
(18 MΩ cm). After drying on air to a stable weight the samples
were subjected to microwave HNO3-assisted (Sigma-Aldrich
Co., St. Louis, MO, USA) degradation in Berghof SW4 sys-
tem (Berghof Products & Instruments, Eningen, Germany) for
20 min at 170–180 °C.
Hair Hg and essential trace element and mineral levels were
evaluated using inductively-coupled plasma mass-
spectrometry at NexION 300D (PerkinElmer Inc., Shelton,
CT, USA) spectrometer equipped with ESI SC-2 DX4
(Elemental Scientific Inc., Omaha, NE, USA) autosampler.
The system was calibrated using Universal Data Acquisition
Standards Kit (PerkinElmer Inc., S helton, CT, USA).
Yttrium-89 and rhodium-103 standard solutions (10 μg/l) pre-
pared from yttrium (Y) and rhodium (Rh) Pure Single-
Element Standard (PerkinElmer Inc.) were used for internal
online standardization. In addition, the certified reference ma-
terial of human hair GBW09101 (Shanghai Institute of
Nuclear Research, Academia Sinica, Taipei, Taiwan, China)
was used for laboratory quality control with the recovery rates
of 87–111%.
The obtained data were processed using Statistica 10.0
software (StatSoft, Tulsa, OK, USA). Shapiro–Wilk test re-
vealed skewed distribution of the laboratory data. Therefore,
medians and interquartile range (IQR) boundaries were used
as descriptive statistics. In view of high variability of demo-
graphic parameters, group comparisons were performed using
analysis of covariance (ANCOVA) with adjustment for age
and gender of examinees with subsequent Bonferroni adjust-
ment. In order to reveal the association between Hg-associated
differences in essential element status and metabolic parame-
ters, multiple linear regression analysis was performed.
Metabolic parameters characterized by significant group dif-
ference (GGT, creatinine, CK, UA) were used as dependent
variables, whereas hair Hg, as well as essential trace element
and mineral levels were considered as independent predictors
in age, gender, and BMI-adjusted models. The level of signif-
icance was set as p < 0.05 for all statistical tests.
Results
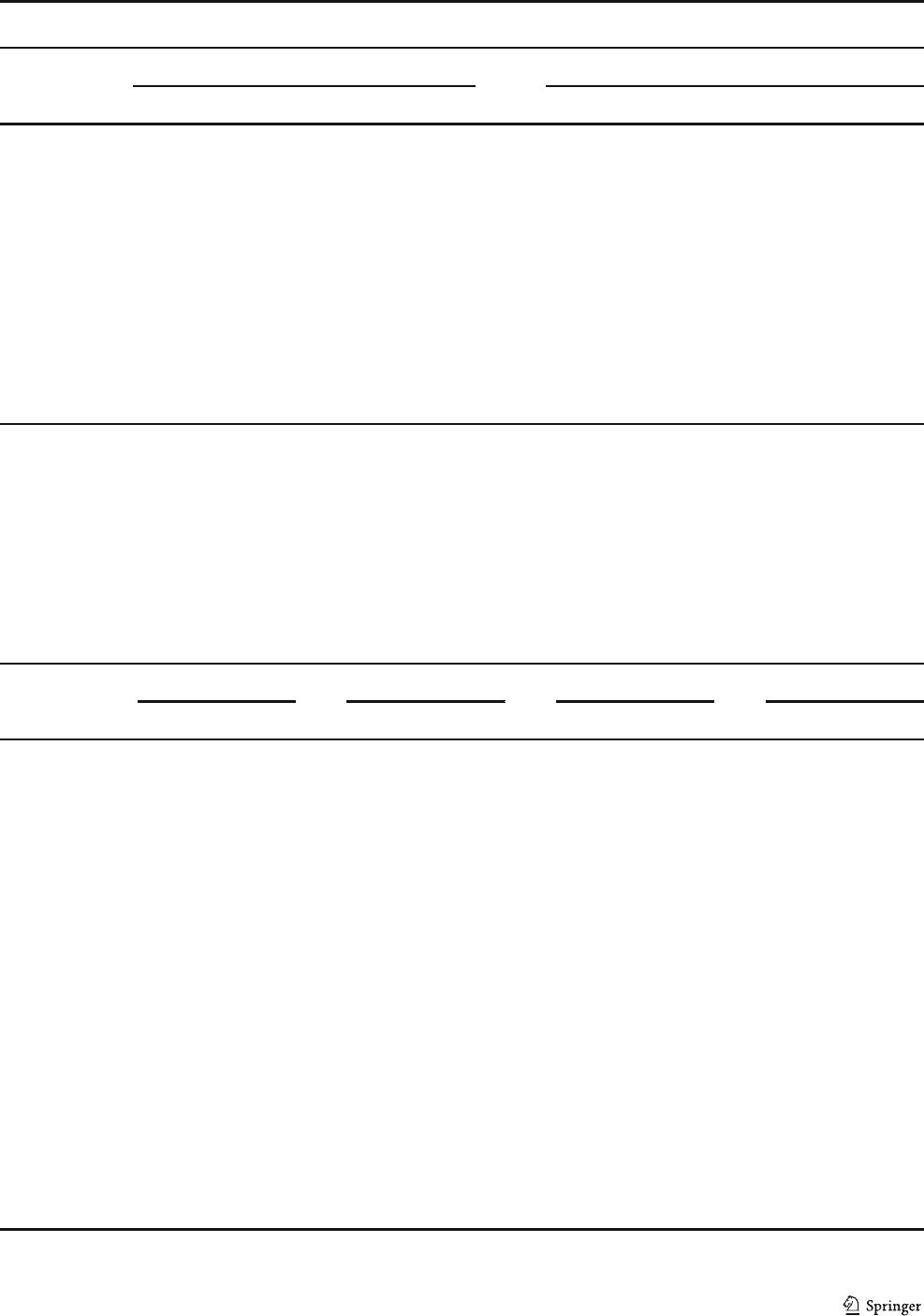
Hair analysis using inductively-coupled plasma demonstrated
that dietary-exposed subjects were characterized by more than
3-fold higher hair Hg content as compared to the respective
body weight groups, in both normal and overweight groups
(Fig. 1).
Table 1 Metabolic risk markers in lean and overweight subjects in relation to hair Hg levels
Parameter Normal weight Overweight and obese
I. Low Hg II. High Hg III. Low Hg IV. High Hg
Age, years 43.99 ± 11.85 43.88 ± 10.53 44.95 ± 12.74 45.85 ± 8.55
Gender (M/F), % 29%/71 25%/75% 34%/66% 36%/64%
BMI, kg/m
2
21.80 ± 1.84 21.81 ± 1.74 28.79 ± 3.40 28.47 ± 3.05
ALT, U/l 17.97 (15.05–24.02) 18.17 (13.91–25.29) 24.67 (17.76–31.05)
1,2
26.53 (20.11–36.31)
1,2
AST, U/l 21.1 (18.26–25.79) 20.18 (17.16–25.3) 21.87 (18.83–25.48) 23.41 (18.19–27.76)
TC, mmol/l 5.14 (4.49–5.65) 5.19 (4.41–6.02) 5.45 (4.67–6.17) 5.11 (4.62–5.88)
Creatinine, μmol/l 81.36 (74.38–89.26) 80.67 (73.22–91.18) 87.11 (74.86–98.23)
2
90.79 (80.25–100.6)
1,2,3
CK, U/l 85.48 (68.81–119.75) 90.25 (65.03–127.38) 98.14 (63.78–148.45) 113.55 (79.64–172.2)
1,2,3
GGT, U/l 12.92 (8.48–20.6) 14.32 (10.46–22.65)
1
20.78 (12.65–34.41)
1,2
25.39 (15.5–37.52)
1,2,3
Glucose, mmol/l 5.16 (4.88–5.44) 5.1 (4.81–5.64) 5.65 (5.14–6.02)
1,2
5.47 (5.14–5.94)
1,2
HDL-C, mmol/l 1.56 (1.33–1.83) 1.62 (1.4–1.91) 1.42 (1.19–1.72)
1,2
1.34 (1.19–1.56)
1,2
LDL-C, mmol/l 2.59 (2.16–3.18) 2.8 (2.1–3.48) 3.24 (2.68–3.95)
1,2
3.26 (2.62–3.72)
1,2
TG, mmol/l 0.78 (0.64–1.08) 0.73 (0.58–0.97) 1.09 (0.78–1.58)
1,2
1.04 (0.81–1.36)
1,2
UA, μmol/l 189.3 (150.1–229.2) 190.4 (154.9–243.3) 259.1 (198.1–311.5)
1,2
277.7 (215.8–313.2)
1,2,3
Urea, mmol/l 4.66 (3.49–6.06) 4.58 (3.95–5.95) 5.17 (4.33–6.28)
1,2
5.4 (4.67–6.65)
1,2,3
Data expressed as median and IQR;
1,2,3
significant group difference in comparison to groups I, II, and III at p < 0.05 according to ANCOVA Bonferroni
post hoc. ALT alanine aminotransferase; AST aspartate aminotransferases; BMI body mass index; CK creatine kinase; GGT gamma-glutamyltransferase;
HDL-C high-density lipoprotein cholesterol; LDL-C low-density lipoprotein cholesterol; TG triglycerides; TC total cholesterol; UA uric acid
Relationship Between Elevated Hair Mercury Levels, Essential Element Status, and Metabolic Profile in...

Differences in both hair Hg content and BMI had a signif-
icant impact on metaboli c parame ters of blood ser um
(Table 1). The obtained data demonstrate that increased hair
Hg levels in normal weight subjects is associated with 11%
higher serum GGT activity as compared to the control sub-
jects. No significant group difference in other metabolic
markers was revealed between high-Hg and low-Hg normal
weight adults.
In contrast to normal weight subjects, high Hg body burden
had a more significant effect on metabolic parameters in over-
weight and obese adults. Particularly, serum creatinine and
uric acid levels in high-Hg overweight examinees exceeded
those in low-Hg overweight counterparts by 4% and 7%, re-
spectively. At the same time, serum creatine kinase and GGT
activity in high-Hg overweight group was 16% and 22%
higher when compared to the respective weight group with
low hair Hg content.
Both low-Hg and high-Hg overweight subjects were char-
acterized by significantly higher ALT activity, as well as ele-
vated serum glucose, LDL-C, and triglyceride levels as com-
pared to the respective groups of normal weight subjects.
High Hg body burden was also associated with significant
differences in hair essential trace element levels (Table 2). In
particular, normal weight high-Hg subjects were characterized
by significantly elevated hair Co, Cu, Se, Si, V, and Zn as
compared to the contro l group by 56%, 11%, 11%, 9%,
67%, and 9%, respectively. In overweight subjects with low
hair Hg content the levels of Ca, Mg, and Zn were found to be
30%, 37%, and 11% lower than those in low-Hg normal
weight controls. More profound differences were observed
in high-Hg overweight group. Specifically, hair Mg levels in
high-Hg overweight subjects were significantly lower than
that in controls and high-Hg normal weight examinees by
49% and 54%, respectively. Hair Mn and Sr concentrations
in high-Hg overweight group compared to low- and high-Hg
lean, and low-Hg obese groups, were lower by 25%, 39%,
22%, and 42%, 43%, 30%, respectively. The highest hair Se
levels were also observed in high-Hg overweight subjects,
being higher than those in groups I, II, and III by 24%, 13%,
and 20%, respectively. It is also notable that the observed 4%
higher Zn levels in high-Hg overweight subjects were signif-
icantly different from low-Hg overweight examinees.
In order to reveal the relative contribution of hair Hg and
essential element levels into the observed difference in GGT,
creatinine, and uric acid, multiple regression analysis was per-
formed (Table 3). After adjustment for age, gender, and BMI
(in all models) hair Hg was considered as a significant predic-
tor only for GGT activity. Hair Cu and Sr levels demonstrated
positive association with serum GGT, whereas hair Mn and
Zn levels were considered as negative predictors of serum
GGT activity. Serum creatinine concentration was inversely
associated with hair Co and Cr content. In turn, hair Fe levels
were positively interrelated with this parameter. Creatine ki-
nase activity was positively and negatively associated with
hair Se and Si levels, respectively. In an adjusted regression
model, hair Cu levels were positively associated with serum
uric acid concentration, whereas hair Si and Zn content was
considered as negative predictor of this parameter. The overall
models accounted for 25%, 33%, 9%, and 40% of GGT, cre-
atinine, CK, and UA variability, respectively.
Discussion
The obtained data demonstrate that Hg-exposed overweight
and obese subjects are characterized by a tendency for higher
metabolic risk as well as altered essential trace element status.
Moreover, Hg-associated differences in essential element sta-
tus were tightly associated with metabolic parameters.
Generally, observed increase in serum glucose, TG, LDL,
and decreased HDL-C levels in overweight low-Hg patients
correspond to the clearly demonstrated association between
obesity, insulin resistance, and atherogenic dyslipidemia. In
turn, elevated GGT and creatine kinase activity, as well as
creatinine and uric acid levels are considered as markers of
metabolic syndrome. Increased ALT activity [33] and urea
[34] concentrations may be indicative of higher risk of nonal-
coholic fatty liver disease in patients with obesity.
At the same time, patients with high hair Hg concentrations
were characterized by more profound increase in serum creat-
inine and uric acid levels, and higher GGT and creatine kinase
activities, thus being indicative of higher metabolic risk.
Recent findings corroborate the earlier data. Particularly, a
significant association between blood Hg levels and increased
GGT activity was demonstrated [35]. Our previous findings
also revealed a positive correlation between hair Hg content
and serum GGT activity [36]. It is also notable that higher Hg
Fig. 1 Hair Hg levels in relation to body weight index and dietary Hg
exposure. Data expressed as median (line), IQR (box), and nonoutlier
range (whiskers). *Significant group difference at p < 0.05 according to
ANCOVA Bonferroni post hoc
Skalny et al.
levels in overweight subjects was associated with elevated
creatinine concertation and creatine kinase levels. Given the
role of these parameters as markers of renal damage [37],
these findings corroborate the existing data on the role of Hg
as a nephrotoxic agent [38], and may be indicative of higher
risk of chronic kidney disease in obesity and metabolic syn-
drome [39]. Serum uric acid levels were also associated with
blood Hg levels in Korean general population [40]. Generally,
Table 3 Multiple regression analysis on the association between metabolic risk markers characterized by significant group differences (dependent
variable) and hair element content (independent variables)
Parameter GGT Creatinine CK UA
β p β p β p β p
Hg 0.122 0.008 * 0.019 0.658 0.025 0.630 0.029 0.484
Ca 0.055 0.413 0.065 0.306 − 0.059 0.424 − 0.056 0.349
Co − 0.033 0.534 − 0.110 0.027 * − 0.017 0.773 − 0.001 0.980
Cr − 0.045 0.344 − 0.135 0.003 * − 0.058 0.267 − 0.007 0.864
Cu 0.131 0.006 * 0.055 0.219 − 0.024 0.642 0.085 0.044 *
Fe 0.040 0.452 0.109 0.030 * 0.034 0.557 − 0.049 0.296
Mg 0.032 0.665 0.033 0.635 − 0.002 0.981 0.119 0.076
Mn − 0.130 0.019 * − 0.008 0.875 0.063 0.297 − 0.090 0.068
Se − 0.057 0.196 0.019 0.653 0.102 0.039 * 0.025 0.530
Si 0.009 0.830 − 0.070 0.083 − 0.124 0.009 * − 0.084 0.028 *
Sr 0.186 0.002 * − 0.020 0.723 − 0.032 0.622 − 0.004 0.946
V − 0.023 0.644 0.087 0.064 0.010 0.858 0.047 0.291
Zn − 0.217 < 0.001 * 0.010 0.835 0.004 0.948 − 0.099 0.026 *
Age 0.312 < 0.001 * 0.555 < 0.001 * 0.263 < 0.001 * 0.478 < 0.001 *
Gender (M/F) 0.146 0.001 * 0.080 0.060 − 0.007 0.882 0.095 0.018 *
BMI 0.231 < 0.001 * 0.062 0.168 − 0.019 0.720 0.260 < 0.001 *
Multiple R 0.527 0.594 0.344 0.650
Multiple R
2
0.277 0.353 0.119 0.423
Adjusted R
2
0.250 0.328 0.085 0.401
p for a model < 0.001 * < 0.001 * < 0.001 * < 0.001 *
Data expressed as regression coefficients (β) and the respective p values; *The association is significant at p <0.05
Table 2 Hair essential trace element and mineral levels in normal weight and overweight adults in relation to hair Hg concentrations (μg/g)
Parameter Normal weight Overweight and obese
I. Low Hg II. High Hg III. Low Hg IV. High Hg
Ca 657.4 (401.9–1414.4) 681.9 (473.8–1314.1) 463.1 (286.3–848.0)
1,2
471.9 (335.1–675.2)
1,2
Co 0.009 (0.005–0.018) 0.014 (0.008–0.034)
1
0.009 (0.005–0.015)
2
0.009 (0.006–0.019)
2
Cr 0.138 (0.072–0.241) 0.176 (0.101–0.295) 0.156 (0.094–0.287) 0.183 (0.097–0.274)
1
Cu 12.96 (10.94–18.44) 14.43 (11.16–25.84)
1
12.27 (9.95–15.69)
2
13.24 (10.6–17.95)
2
Fe 11.62 (8.77–17.89) 12.06 (8.89–17.95) 11.88 (8.26–15.8) 10.97 (8.34–16.19)
2
Mg 83.42 (41.62–158.08) 92.44 (45.78–166.08) 52.85 (25.27–127.33)
1,2
42.57 (25.22–69.35)
1,2,3
Mn 0.388 (0.256–0.807) 0.411 (0.247–0.861) 0.373 (0.215–0.68) 0.291 (0.194–0.476)
1,2,3
Se 0.358 (0.281–0.487) 0.392 (0.317–0.499)
1
0.370 (0.269–0.493) 0.444 (0.308–0.574)
1,2,3
Si 16.04 (10.61–20.75) 17.55 (12.58–24.24)
1
17.17 (12–23.9) 15.33 (11.98–20.83)
Sr 2.182 (1.026–4.696) 2.195 (0.962–4.83) 1.802 (0.726–5.701) 1.270 (0.687–2.59)
1,2,3
V 0.009 (0.006–0.019) 0.015 (0.009–0.034)
1
0.012 (0.007–0.020)
2
0.010 (0.007–0.019)
2
Zn 194.0 (163.2–228.3) 210.7 (181.7–246.1)
1
171.9 (137.0–205.2)
1,2
178.5 (152.8–215.3)
2,3
Data expressed as median and IQR;
1,2,3
Significant group difference in comparison to groups 1, 2, and 3 at p < 0.05 according to ANCOVA Bonferroni
post hoc
Relationship Between Elevated Hair Mercury Levels, Essential Element Status, and Metabolic Profile in...

these obtained data corroborate findings by Lee [14] who
demonstrated adverse metabolic profile and tendency for met-
abolic unhealthy obesity with increased blood Hg levels.
In the present study, analysis of hair essential trace element
and mineral content demonstrated that overweight and obesity
were associated with significantly reduced Ca, Mg, and Zn
levels when compared to normal weight controls.
The observed levels of Ca in hair of overweight subjects
generally correspond to the earlier finding of lower Ca intake
in obesity [40, 41]. Experimental data also demonstrated that
low Ca intake is associated with higher susceptibility to diet-
induced obesity [42] and associated metabolic disturbances
[43]. Generally, the relationship between obesity and Ca me-
tabolism may be mediated by the role of the latter in regulation
of adipogenesis, lipid metabolism, thermogenesis, and gut mi-
crobiota [44]. It is also notable that the relationship between
Ca and obesity may be mediated by vitamin D [45].
Recent data demonstrate significantly reduced intracellular
Mg levels in subjects with obesity and diabetes [46], being in
agreement with our findings. Correspondingly, Mg intake is
known to be inversely associated with obesity and metabolic
syndrome [47]. In addition, low Mg levels is known to be
associated with adverse metabolic profile in obesity [48].
Antiinflammatory, antioxidant, hypolipidemic, as well as
insulin-sensitizing effects of Mg may underlie the observed
differences [20, 49].
Similarly, Zn deficiency was shown to be a frequent find-
ing in overweight and obese subjects [23], being related to
obesity-associated metabolic disturbances including dyslipid-
emia, insulin resistance, and hypertension [50]. In turn, Zn
supplementation was reported to improve metabolic status in
obese subjects [51]. A close association between zinc, obesity,
and metabolic syndrome is mediated by the role of Zn in
insulin secretion and signaling, adipogenesis and adipocyte
functioning, lipi d metabolism, as well as antioxid ant and
antiinflammatory effect [16].
Along with more profound alterations of metabolic param-
eters in overweight subjects, Hg exposure was associated with
aberrant essential trace element profile in hair. Particularly, Hg
exposure aggravated overweight-associated decrease in hair
Mg content. Experimental data demonstrated that methylmer-
cury exposure significantly reduced kidney and spleen Mg
levels in rats [26]. These effects may result from competitive
binding of Hg
2+
to Mg-containing enzymes [24].
Although no further decrease in hair Zn levels were ob-
served in Hg-exposed overweight subjects, h igh hair Hg
levels were associated with elevation of hair Zn that may be
also indicative of Hg-induced alterations in Zn metabolism.
Correspondingly, inorganic Hg exposure was shown to in-
crease kidney Zn levels in vivo [26]. At the same time, zinc
treatment may counteract Hg-induced metabolic disturbances
including altered ALT activity, as well as urea, creatinine, and
glucose levels [52], whereas Zn-induced metallothionein
production may reduce tissue Hg deposition thus preventing
its adverse effects [53].
It is also notable that dietary Hg exposure in the overweight
group led to increased hair Cr levels. Despite a significant
increase in hair Cr levels in high-Hg overweight subjects,
these findings may be indicative of lower serum Cr levels as
demonstrated in the study of paired hair-serum-urine samples
in obese examinees [54]. However, the particular mechanisms
of Hg-induced alterations of Cr homeostasis were not estimat-
ed. Given the role of Cr as insulin signaling and adipose tissue
physiology [17], one can propose that altered Cr metabolism
may significantly contribute to obesity-associated metabolic
disorders, especially in high-Hg group.
TheobserveddecreaseinhairMnlevelsinoverweightHg-
exposed subjects generally corresponds to the results of an
earlier in vivo study demonstrating a significant reduction in
hepatic Mn levels in methylmercury-exposed rats due to Hg-
induced arginase I inhibition and Mn
2+
release [55]. In turn,
Mn was also shown to be involved in metabolic syndrome
pathogenesis through its interference with redox homeostasis,
lipid and carbohydrate metabolism [56].
Increased hair Hg content was associated with elevated hair
Se levels both in normal weight and overweight subjects. Se is
known to be Hg antagonist acting through a variety of mecha-
nisms including direct chemical interaction with the formation
of Hg-Se compounds that are excreted from the organism [25]
that may underlie a direct relationship between these elements
in hair. In addition, given the primary role of seafood intake in
elevated hair Hg content, this dietary pattern may also underlie
higher hair Se levels due to the role of sea fish as a dietary
source of Se [57]. At the same time, Hg-associated increase in
hair Se content was more profound in overweight group, being
in agreement with our observation of higher body Se burden in
obese subjects [54]. Se was also shown to modify the associa-
tionbetweenmercuryandmetabolic syndrome [58].
The obtained data correspond well to the role of seafood
consumption as the source of mercury [13]. At the same time,
seafood intake also contributes significantly to exposure to
polychlorinated biphenyls and organochlorine pesticides
[59] that are considered as potent obesogens and promotors
of metabolic syndrome due to endocrine disruption [60].
Therefore, the observation of adverse metabolic profile in sea-
food consumers may be at least partially mediated by organic
obesogens.
Generally, the obtained data demonstrate that increased
hair Hg levels in overweight and obese subjects is associated
with adverse metabolic profile. It is proposed that observed
metabolic alterations may be at least partially mediated by Hg-
associated disturbances in essential trace element and mineral
metabolism. However, further laboratory and epidemiological
studies are required to unravel the relationship between Hg
exposure and trace element and mineral metabolism in obesity
and its impact on metabolic syndrome pathogenesis.
Skalny et al.

Funding The study was supported by grants No. 20-515-S52003 from
the Russian Foundation for Basic Research (Russia) and MOST 109-
2923-B-038-001-MY3 from the Ministry of Science and Technology
(Taiwan).
Compliance with Ethical Standards
Conflict of Interest The authors declare that they haave no conflict of
interest.
References
1. Organisation for Economic Co-operation and Development.
Obesity update 2017. OECD https://www.oecd.org/els/health-
systems/Obesity-Update-2017.pdf (2017)
2. Blüher M (2019) Obesity: global epidemiology and pathogenesis.
Nat Rev Endocrinol 15(5):288–298. https://doi.org/10.1038/
s41574-019-0176-8
3. Baillie-Hamilton PF (2002) Chemical toxins: a hypothesis to ex-
plain the global obesity epidemic. J Altern Complement Med 8(2):
185–192. https://doi.org/10.1089/107555302317371479
4. Nappi F, Barrea L, Di Somma C, Savanelli MC, Muscogiuri G,
Orio F, Savastano S (2016) Endocrine aspects of environmental
“Obesogen” pollutants. Int J Environ Res Public Health 13(8):
765. https://doi.org/10.3390/ijerph13080765
5. Wang X, Mukherjee B, Park SK (2018) Associations of cumulative
exposure to heavy metal mixtures with obesity and its comorbidities
among U.S. adults in NHANES 2003-2014. Environ Int 121(Pt 1):
683–694. https://doi.org/10.1016/j.envint.2018.09.035
6. Heindel JJ (2019) History of the Obesogen field: looking back to
look forward. Front Endocrinol (Lausanne) 10:14. https://doi.org/
10.3389/fendo.2019.00014
7. Skalnaya MG, Tinkov AA, Demidov VA, Serebryansky EP,
Nikonorov AA, Skalny AV (2014) Hair toxic element content in
adult men and women in relation to body mass index. Biol Trace
Elem Res 161(1 ):13–19. https://doi.org/10 .1007/s12011 -014-
0082-9
8. Shin YY, Ryu IK, Park MJ, Kim SH (2018) The association of total
blood mercury levels and overweight among Korean adolescents:
analysis of the Korean National Health and Nutrition Examination
Survey (KNHANES) 2010-2013. Korean J Pediatr 61(4):121–128.
https://doi.org/10.3345/kjp.2018.61.4.121
9. Park JS, Ha KH, He K, Kim DJ (2017) Association between blood
mercury level and visceral adiposity in adults. Diabetes Metab J
41(2):113–120. https://doi.org/10.4093/dmj.2017.41.2.113
10. Eom SY, Choi SH, Ahn SJ, Kim DK, Kim DW, Lim JA, Choi BS,
Shin HJ, Yun SW, Yoon HJ, Kim YM, Park K, Seo E (2016)
Association between toenail mercury and metabolic syndrome is
modified by selenium. Nutrients 8(7):424. https://doi.org/10.3390/
nu8070424
11. Rothenberg SE, Korrick SA, Fayad R (2015) The influence of
obesity on blood mercury levels for U.S. non-pregnant adults and
children: NHANES 2007-2010. Environ Res 138:173–180. https://
doi.org/10.1016/j.envres.2015.01.018
12. Tinkov AA, Ajsuvakova OP, Skalnaya MG, Popova EV, Sinitskii
AI, Nemereshina ON, Gatiatulina ER, Nikonorov AA, Skalny AV
(2015) Mercury and metabolic syndrome: a review of experimental
and clinical observations. Biometals 28(2):231–254. https://doi.org/
10.1007/s10534-015-9823-2
13. Roy C, Tremblay PY, Ayotte P (2017) Is mercury exposure causing
diabetes, metabolic syndrome and insulin resistance? A systematic
review of the literature. Environ Res 156:747–760. https://doi.org/
10.1016/j.envres.2017.04.038
14. Lee K (2018) Blood mercury concentration in relation to metabolic
and weight phenotypes using the KNHANES 2011-2013 data. Int
Arch Occup Environ Health 91(2):185–193. https://doi.org/10.
1007/s00420-017-1269-0
15. Wiernsperger N, Rapin J (2010) Trace elements in glucometabolic
disorders: an update. Diabetol Metab Syndr 2:70. https://doi.org/10.
1186/1758-5996-2-70
16. Olechnowicz J, Tinkov A, Skalny A, Suliburska J (2018) Zinc
status is associated with inflammation, oxidative stress, lipid, and
glucose metabolism. J Physiol Sci 68(1):19–31. https://doi.org/10.
1007/s12576-017-0571-7
17. Vincent JB (2019) Effects of chromium supplementation on body
composition, human and animal health, and insulin and glucose
metabolism. Curr Opin Clin Nutr Metab Care 22(6):483–489.
https://doi.org/10.1097/MCO.0000000000000604
18. Treviño S, Diaz A (2020) Vanadium and insulin: partners in meta-
bolic regulation. J Inorg Biochem 208:111094. https://doi.org/10.
1016/j.jinorgbio.2020.111094
19. Tinkov AA, Ajsuvakova OP, Filippini T, Zhou JC, Lei XG,
Gatiatulina ER, Michalke B, Skalnaya MG, Vinceti M, Aschner
M, Skalny AV (2020) Selenium and selenoproteins in adipose tis-
sue physiology and obesity. Biomolecules 10(4):658. https://doi.
org/10.3390/biom10040658
20. Nielsen FH (2018) Magnesium deficiency and increased inflamma-
tion: current perspectives. J Inflamm Res 11:25–34. https://doi.org/
10.2147/JIR.S136742
21. Astrup A, Bügel S (2010) Micronutrient deficiency in the aetiology
of obesity. Int J Obes 34(6):947–948. https://doi.org/10.1038/ijo.
2010.81
22. Via M (2012) The malnutrition of obesity: micronutrient deficien-
cies that promote diabetes. ISRN Endocrinol 2012:103472–
103478. https://doi.org/10.5402/2012/103472
23. Gu K, Xiang W, Zhang Y, Sun K, Jiang X (2019) The association
between serum zinc level and overweight/obesity: a meta-analysis.
Eur J Nutr 58(8):2971–2982. https://doi.org/10.1007/s00394-018-
1876-x
24. Ynalvez R, Gutierrez J, Gonzalez-Cantu H (2016) Mini-review:
toxicity of mercury a s a consequence o f enz yme alterati on.
Biometals. 29(5):781–788. https://doi.org/10.1007/s10534-016-
9967-8
25. Bjørklund G, Aaseth J, Ajsuvakova OP, Nikonorov AA, Skalny
AV, Skalnaya MG, Tinkov AA (2017) Molecular interaction be-
tween mercury and selenium in neurotoxicity. Coord Chem Rev
332:30–37. https://doi.org/10.1016/j.ccr.2016.10.009
26. Bogden JD, Kemp FW, Troia no RA, Jortner BS, Timpone C,
Giuliani D (1980) Effect of mercuric chloride and methylmercury
chloride exposure on tissue concentrations of six essential minerals.
Environ R es 21(2):350–359. h ttps://doi.org/10.10 16/0013-
9351(80)90037-7
27. Feng W, Wang M, Li B, Liu J, Chai Z, Zhao J, Deng G (2004)
Mercury and trace element distribution in organic tissues and re-
gional brain of fetal rat after in utero and weaning exposure to low
dose of inorganic mercury. Toxicol Lett 152(3):223–234. https://
doi.org/10.1016/j.toxlet.2004.05.001
28. Trasande L, DiGangi J, Evers DC, Petrlik J, Buck DG, Šamánek J,
Beeler B, Turnquist MA, Regan K (2016) Economic implications
of mercury exposure in the context of the global mercury treaty: hair
mercury levels and estimated lost economic productivity in selected
developing countries. J Environ Manag 183:229–235. https://doi.
org/10.1016/j.jenvman.2016.08.058
29. Kim HR, Han MA (2018) Association between serum liver en-
zymes and metabolic syndrome in Korean adults. Int J Environ
Res Public Health 15(8):1658. https://doi.org/10.3390/
ijerph15081658
30. Lee DS, Evans JC, Robins SJ, Wilson PW, Albano I, Fox CS,
Wang TJ, Benjamin EJ, D' Agostino RB, Vasan RS (2007)
Relationship Between Elevated Hair Mercury Levels, Essential Element Status, and Metabolic Profile in...

Gamma glutamyl transferase and metabolic syndrome, cardiovas-
cular disease, and mortality risk: the Framingham Heart Study.
Arterioscler Thromb Vasc Biol 27(1):127–133. https://doi.org/10.
1161/01.ATV.0000251993.20372.40
31. Wang J, Li X, Han X, Yang K, Liu B, Li Y, Wu P, Liu X, Yu K, Dai
X, Yuan J, Yao P, Zhang X, Guo H, Wang Y, Chen W, Wei S,
Miao X, Min X, Liang Y, Yang H, Hu FB, Wu T, He M (2015)
Serum creatinine levels and risk of metabolic syndrome in a middle-
aged and older Chinese population. Clin Chim Acta 440:177–182.
https://doi.org/10.1016/j.cca.2014.11.025
32. Yang T, Chu CH, Bai CH, You SL, Chou YC, Chou WY, Chien
KL, Hwang LC, Su TC, Tseng CH, Sun CA (2012 Feb) Uric acid
level as a risk marker for metabolic syndrome: a Chinese cohort
study. Atherosclerosis. 220(2):525–531. https://doi.org/10.1016/j.
atherosclerosis.2011.11.014
33. Chen ZW, Chen LY, Dai HL, Chen JH, Fang LZ ( 2008)
Relationship between alanine aminotransferase levels and metabol-
ic syndrome in nonalcoholic fatty liver disease. J Zhejiang Univ Sci
B9(8):616–622. https://doi.org/10.1631/jzus.B0720016
34. Liu X, Zhang H, Liang J (2013) Blood urea nitrogen is elevated in
patients with non-alcoholic fatty liver disease.
Hepatogastroenterology 60(122):343–345
35. Seo MS, Lee HR, Shim JY, Kang HT, Lee YJ (2014) Relationship
between blood mercury concentrations and serum γ -
glutamyltranspeptidase level in Korean adults using data from the
2010 Korean National Health and Nutrition Examination Survey.
Clin Chim Acta 430:160–163. https://doi.org/10.1016/j.cca.2014.01.
042
36. Tinkov AA, Skalnaya MG, Demido v VA, Serebryansky EP,
Nikonorov AA, Skalny AV (2014) Hair mercury association with
selenium, serum lipid spectrum, and gamma-glutamyl transferase
activity in adults. Biol Trace Elem Res 161(3):255–262. https://doi.
org/10.1007/s12011-014-0124-3
37. Gowda S, Desai PB, Kulkarni SS, Hull VV, Math AA, Vernekar
SN (2010) Markers of renal function tests. N Am J Med Sci 2(4):
170–173
38. Bridges CC, Zalups RK (2017) The aging kidney and the nephro-
toxic effects of mercury. J Toxicol Environ Health B Crit Rev
20(2):55–80. https://doi.org/10.1080/10937404.2016.1243501
39. Chen J, Gu D, Chen CS, Wu X, Hamm LL, Muntner P, Batuman V,
Lee CH, Whelton PK, He J (2007) Association between the meta-
bolic syndrome and chronic kidney disease in Chinese adults.
Nephrol Dial Transplant 22(4):1100–1106. https://doi.org/10.
1093/ndt/gfl759
40. Schrager S (2005) Dietary calcium intake and obesity. J Am Board
Fam Pract 18(3):205–210. https://doi.org/10.3122/jabfm.18.3.205
41. Skowrońska-Jóźw iak E, Jawo rski M, Lo renc R, K arbownik -
Lewińska M, Lewiński A (2017) Low dairy calcium intake is as-
sociated with overweight and elevated blood pressure in Polish
adults, notably in p remenopausal women. Public Health Nutr
20(4):630–637. https://doi.org/10.1017/S1368980016002706
42. He YH, Li ST, Wang YY, Wang G, He Y, Liao XL, Sun CH, Li Y
(2012) Postweaning low-calcium diet promotes later-life obesity
induced by a high-fat diet. J Nutr Biochem 23(10):1238–1244.
https://doi.org/10.1016/j.jnutbio.2011.07.004
43. Marotte C, Bryk G, Gonzales Chaves MM, Lifshitz F, de Portela
ML, Zeni SN (2014) Low dietary calcium and obesity: a compara-
tive study in genetically obese and normal rats during early growth.
Eur J Nutr 53(3):769–778. https://doi.org/10.1007/s00394-013-
0581-z
44. Zhang F, Ye J, Zhu X, Wang L, Gao P, Shu G, Jiang Q, Wang S
(2019) Anti-obesity effects of dietary calcium: the evidence and
possible mechanisms. Int J Mol Sci 20(12):3072. https://doi.org/
10.3390/ijms20123072
45. Pannu PK, Calton EK, Soares MJ (2016) Calcium and vitamin D in
obesity and related chronic disease. Adv Food Nutr Res 77:57–100.
https://doi.org/10.1016/bs.afnr.2015.11.001
46. Takaya J, Yamato F, Kuroyanagi Y, Higashino H, Kaneko K
(2010) Intracellular magnesium of obese and type 2 diabetes
mellitus children. Diabetes Ther 1(1):25–31. https://doi.org/10.
1007/s13300-010-0003-7
47 . Sarrafzadegan N, Khosravi-Boroujeni H , Lotfizadeh M,
Pourmogaddas A, Salehi-Abargouei A (2016) Magnesium status and
the metabolic syndrome: a systematic review and meta-analysis.
Nutrition 32(4):409–417. https://doi.org/10.1016/j.nut.2015.09.014
48. Guerrero-Romero F, Rodriguez-Moran M (2013) Serum magne-
sium in the metabolically-obese normal-weight and healthy-obese
subjects. Eur J Intern Med 24(7):639–643. https://doi.org/10.1016/
j.ejim.2013.02.014
49. Volpe SL (2013) Magnesium in disease prevention and overall
health. Adv Nutr 4(3):378S–383S. https://doi.org/10.3945/an.112.
003483
50. Freitas EP, Cunha AT, Aquino SL, Pedrosa LF, Lima SC, Lima JG,
Almeida MG, Sena-Evangelista KC (2017) Zinc status biomarkers
and cardiometabolic risk factors in metabolic syndrome: a case
control study. Nutrients 9(2):175. https://doi.org/10.3390/
nu9020175
51. Kim J, Ahn J (2014) Effect of zinc supplementation on inflamma-
tory markers and adipokines in young obese women. Biol Trace
Elem Res 157(2):101–106. https://doi.org/ 10.1007/s12011-013-
9885-3
52. Franciscato C, Moraes-Silva L, Duarte FA, Oliveira CS, Ineu RP,
Flores EM, Dressler VL, Peixoto NC, Pereira ME (2011) Delayed
biochemical changes induced by mercury intoxication are
prevented by zinc pre-exposure. Ecotoxicol Environ Saf 74(3):
480–486. https://doi.org/10.1016/j.ecoenv.2010.11.011
53. Peixoto NC, Serafim MA, Flores EM, Bebianno MJ, Pereira ME
(2007) Metallothionein, zinc, and mercury levels in tissues of
young rats exposed to zinc and subsequently to mercury. Life Sci
81(16):1264–1271. https://doi.org/10.1016/j.lfs.2007.08.038
54. Tinkov AA, Skalna ya MG, Ajsuvakova OP, Serebryansky EP,
Chao JC, Aschner M, Skalny AV (2020) Selenium, zinc, chromi-
um, and vanadium levels in serum, hair, and urine samples of obese
adults assessed by inductively coupled plasma mass spectrometry.
Biol Trace Elem Res 1-8. https://doi.org/10.1007/s12011-020-
02177-w.
55. Kanda H, Sumi D, Endo A, Toyama T, Chen CL, Kikushima M,
Kumagai Y (2008) Reduction of arginase I activity and manganese
levels in the liver during exposure of rats to methylmercury: a
possible mechanism. Arch Toxicol 82(11):803–808. https://doi.
org/10.1007/s00204-008-0307-9
56. Li L, Yang X (2018) The essential element manganese, oxidative
stress, and metabolic diseases: links and interactions. Oxidative
Med Cell Longev 2018:7580707–7580711. https://doi.or g/10.
1155/2018/7580707
57. Yamashita Y, Yamashita M, Iida H (2013) Selenium content in
seafood in Japan. Nutrients 5(2):388–395. https://doi.org/10.3390/
nu5020388
58. Park K, Seo E (2016) Association between toenail mercury and
metabolic syndrome is modified by selenium. Nutrients 8(7):424
59. Qian Z, Luo F, Wu C, Zhao R, Cheng X, Qin W (2017) Indicator
polychlorinated biphenyls (PCBs) and organochlorine pesticides
(OCPs) in seafood from Xiamen (China): levels, distributions, and
risk assessment. Environ Sci Pollut Res 24:10443–10453
60. Heindel JJ, Blumberg B (2019) Environmental obesogens: mecha-
nisms and controversies. Annu Rev Pharmacol Toxicol 59:89–106
Publisher’sNoteSpringer Nature remains neutral with regard to jurisdic-
tional claims in published maps and institutional affiliations.
Skalny et al.
